Inside Bethsaida Healthcare’s accelerated digital transformation strategy
)
Bethsaida Hospital Serang has received EMRAM Stage 6 certification, driving clinical quality and operational efficiency.
Indonesia’s Bethsaida Hospital Serang (BHS) marked a significant milestone in its digital transformation journey with its validation for Stage 6 of HIMSS’ Electronic Medical Record Adoption Model (EMRAM). EMRAM measures EMR maturity from Stages 0 to 7, with Stage 6 indicating advanced capabilities in clinical documentation, data exchange, and interoperability.
 |
Receiving this certification as a relatively new facility – BHS began operations in August 2024 – is no easy feat. The accelerated progress was made possible because the hospital was envisioned as a smart hospital right from its conceptualisation, said Hasan Widjaja, Chief Technology Officer at Bethsaida Healthcare. Mr Hasan oversees digital strategy and governance across Bethsaida Healthcare’s networks, which include two hospitals – Bethsaida Hospital Serang and Bethsaida Hospital Gading Serpong – and three clinics. |
“Our digital strategy was built with four main objectives in mind: to improve patient experience and user experience, smoothen business processes, and enable data-driven analytics,” he shared.
“To support these goals, we developed a holistic IT roadmap spanning across infrastructure, application, mobile access, AI & IoT, and data.”
EMR as the backbone of transformation
BHS was built as a paperless hospital, with all documentation and data exchange conducted within the EMR platform.
The system is connected to numerous medical equipment, such as blood pressure and heart rate monitors, for real-time monitoring of patient conditions. For ICU patients who require close attention, clinicians can access their vital signs and key health metrics directly on their mobile devices, enabling swift and timely interventions as needed.
The hospital shares a unified EMR with its sister facility in Gading Serpong, ensuring digital standardisation and data integration across hospital units. Plans are underway to bring the group’s clinics onboard the system as well.

Cutting discharge waiting times through digital workflows
Having a solid digital infrastructure allows the hospital to explore customised modules targeting specific operational and clinical challenges.
One such initiative focuses on enhancing patient discharge coordination.
“One of the primary concerns for inpatients is discharge waiting time. Based on our studies and observations, delays were caused by several factors, including time taken to process discharge instructions from doctors, medication preparation, and payment. The processes relied heavily on the nurses: they were responsible for informing and coordinating between various hospital units for every single discharge,” Mr Hasan shared.
Discharge coordination has since been automated through the Patient Discharge Monitoring system launched in 2024. When doctors initiate a discharge in the system, it automatically generates notifications to all relevant units. Progress can be monitored through a dashboard, improving transparency and accountability across units.
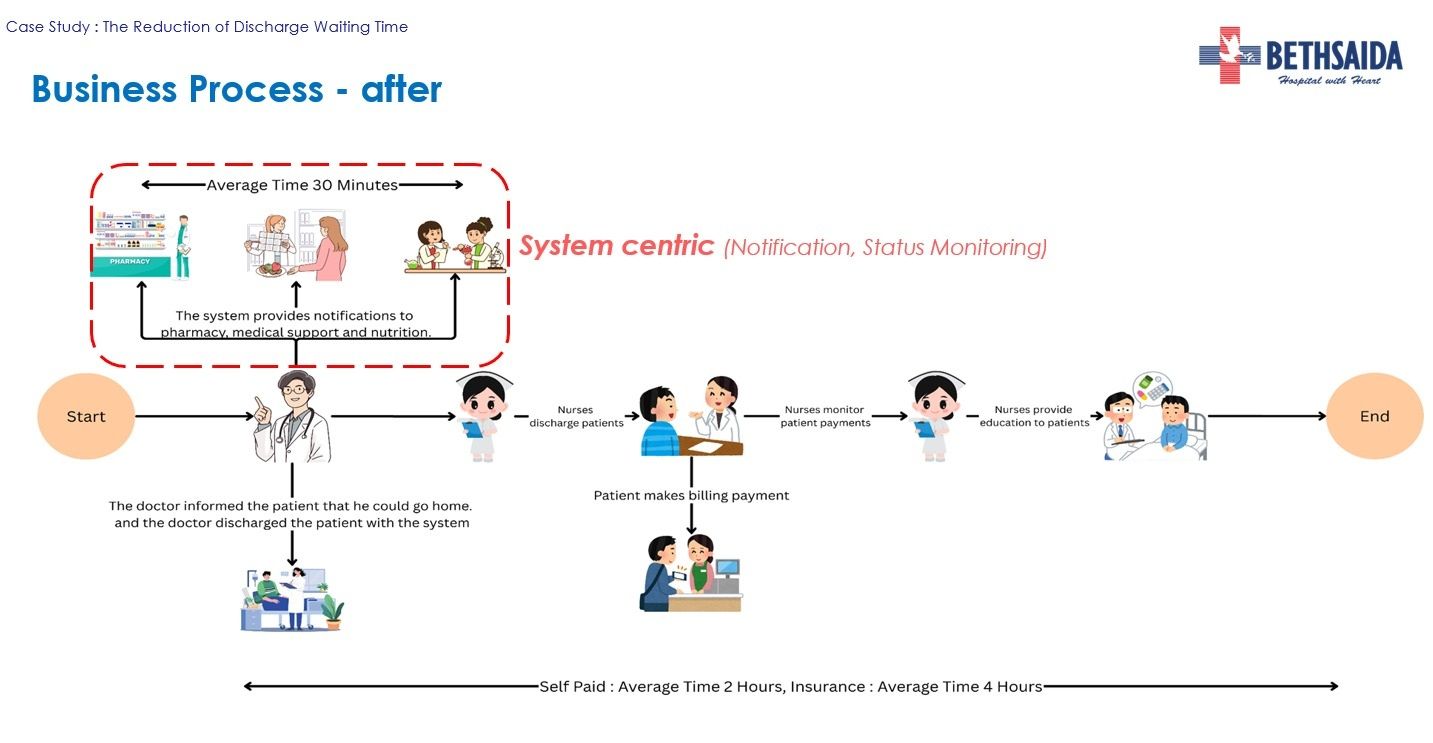
Patients also receive automated status updates via WhatsApp.
“By keeping patients updated on the progress and the estimated waiting times, we manage their expectations and reduce uncertainty,” Mr Hasan explained.
The system has delivered impressive results so far. Average discharge waiting times for insured patients fell from 6.3 hours to 2.9 hours. For self-pay patients, waiting times slid from 3.1 hours to 2.1 hours. Patient satisfaction with their discharges rose in tandem, from 81% in November 2024 to over 96% in April 2025.
Operationally, faster discharge processing has also improved VIP room turnover, contributing to higher room utilisation rates and increased revenue.

The next phase in Bethsaida Hospitals’ digitalisation roadmap
Artificial intelligence (AI) is set to play a bigger role in Bethsaida’s upcoming digital transformation plans.
The group has already introduced AI-powered search in the EMR, allowing clinicians to retrieve information through natural language queries (for example, “What was the last drug prescribed to the patient?”) – drastically reducing search time. This functionality similarly benefits administrative units in retrieving data for reporting and analytics.
The team is also exploring new relevant AI applications, for example in patient health analysis. Of interest is also the use of virtual reality (VR) to reduce patient anxiety, particularly amongst paediatric patients. An immersive VR environment that provides distraction and comfort to patients during procedures could support treatment adherence and recovery outcomes.
Another item on his agenda this year is creating a back-up of hospital data on cloud, to mitigate the risk of downtime during network disruption.
Finally, he is keeping a close eye on wearable technologies, and how the hospital can leverage these in continuous monitoring and chronic disease management.
As the technology continues to advance rapidly, a growing range of wearables could be integrated with EMR systems. When patients’ readings exceed certain thresholds, the system could alert clinicians to follow up and take preventive measures before their condition worsens.
“We will continue strengthening our digital ecosystem and investing in technologies that respond to patient needs,” Mr Hasan concluded. “Our focus is on adopting innovations that support safer, more responsive, and higher-quality care for the communities we serve.”

